In these times of fewer conventions, congresses, and scientific meetings the world is luckily still continuing scientific research and publishing their results. A group of chemists recently published a review on the resistance of mature biofilms to antimicrobial agents. The capability of biofilms to protect and preserve themselves has received great attention in the literature in recent years as they are considered multi-drug-resistant “superbugs”. Li et al. has described in the journal of the American Chemical society the clinical context of this issue.
Biofilms, described here as aggregations of microorganisms living in an extracellular matrix, are very often resistant to antibiotics in a mature state. In fact, in biofilm-related infections, biofilm-growing cells are resistant not only to conventional antibiotic treatment but also to the host’s immune system, causing the recurrence and recalcitrance of the infection.
In 2017, Schultz et al. stated that there is a growing consensus that biofilms contribute to a delay in the healing of chronic wounds and that there is increasing evidence that biofilms are present in most, if not all, chronic nonhealing wounds. A meta-analysis of in vivo studies has found that at least 78% of chronic wounds contain a biofilm, revealing the medical importance of solutions that is able to effectively battle the biofilm in chronic wounds.
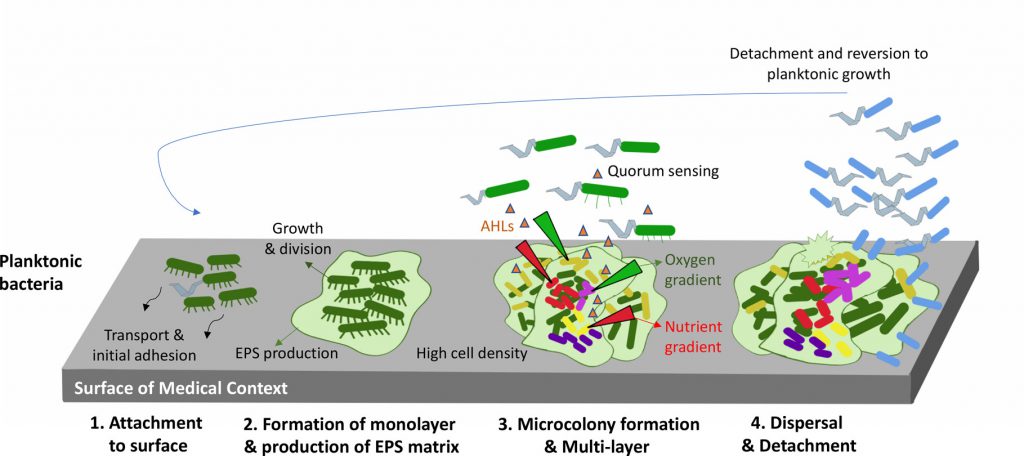
Li et al have described the biofilm attachment, formation, and detachment process as follows: It begins with (i) the transport and initial adhesion of the planktonic bacteria through the adsorption of suspended particles and organic species from the bulk fluid, (ii) transport and attachment of the planktonic cells, (iii) microbial multiplication and EPS production (natural polymers of high molecular weight secreted by microorganisms into their environment), and (iv) dispersal and detachment of the mature clusters.
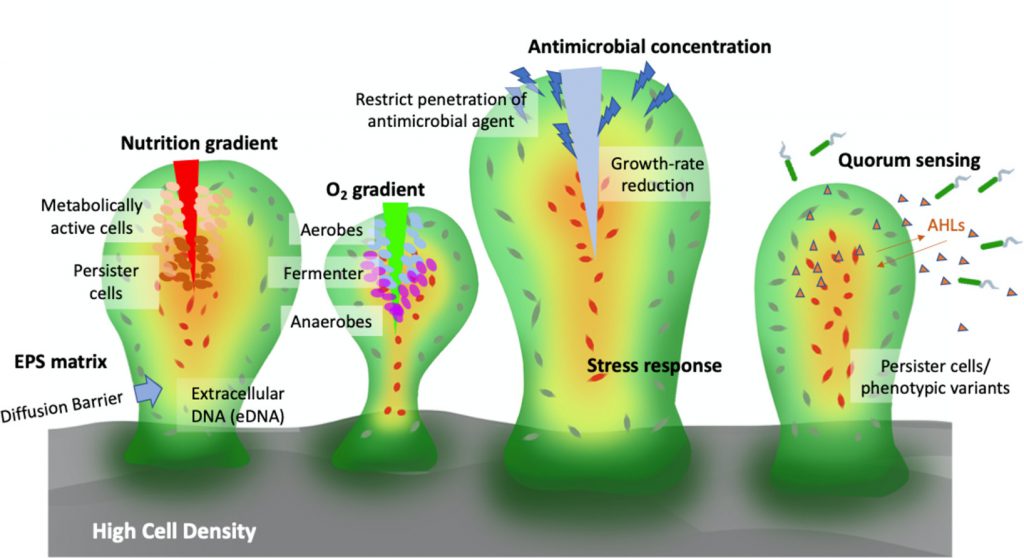
Some of the given reasons behind biofilms being multi-drug-resistant “superbugs” are the high bacterial density in the biofilm, the metabolic activities of the bacteria in the biofilm and the extracellular polymeric substances that form a protective barrier. The bacterial density prevents antibiotic agents from reaching the entire thickness of the biofilm. The high metabolic rate also removes these agents in a rapid speed. In addition, the polymeric substances in the extracellular spaces form a protective layer that keeps the antibiotic agents from penetrating to the core of the biofilm. This keeps the biofilm intact and difficult to treat.
The article of Li et al. proposes to resolve this issue with a combination of therapies, either a combination of different antibiotics or antibiotics with compounds that can disrupt the biofilm matrix. However, looking at the fact that also the bacteria inside the biofilm can become resistant to antibiotics over time, a solution to battle biofilms that does not include any antibiotics would be even better.
Curious to the solution DEBx Medical proposes to battle the biofilm in infected chronic wounds? Visit our product page to learn all about DEBRICHEM or get in touch with our representatives via our contact page!
Article can be found: https://pubs.acs.org/doi/10.1021/acsomega.0c02294